Cannabinoid Hyperemesis Syndrome
Cannabinoid Hyperemesis Syndrome (CHS) is an often under-recognized condition that leads to repeated and severe bouts of vomiting. The disease was relatively rare, but since cannabis is now medically prescribed in Florida, the syndrome is being seen in the ERs more frequently. Cannabinoid hyperemesis syndrome occurs in daily long-term users of marijuana (cannabis). Usually, marijuana and other cannabinoids decrease nausea and vomiting, but in some long-term high-frequency users, marijuana has the opposite effect.
Etiology and Pathophysiology:
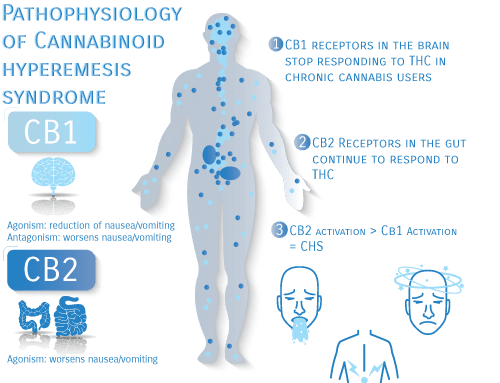
Δ9 -tetrahydrocannabinol (THC) activates CB1 and CB2 receptors in the body. When the CB1 receptor in the brain is activated or “turned on,” nausea and vomiting symptoms are mitigated. CB2 receptor activation in the intestines (gut) has the opposite effect (worsens nausea/vomiting). Initially, THC activates CB1 > CB2, thus providing the anti-emetic (anti-nausea) relief. This is why THC is used for chemotherapy-induced nausea and vomiting (CINV). However, in chronic THC users, the CB1 receptor becomes “desensitized.” The CB1 receptors in specific parts of the brain stop responding to the THC while the CB2 receptors in the gut remain functional. Therefore, THC activates CB2>CB1 and worsens the gastrointestinal symptoms (thus causing Cannabinoid Hyperemesis Syndrome). The exact cause of why the CB1 doesn’t respond as well to THC is not known.
Diagnosis:
Before Cannabinoid Hyperemesis Syndrome is confirmed, the standard of care is to rule out other gastrointestinal (GI) conditions. CHS is often confused with cyclical vomiting syndrome or psychogenic vomiting. The typical work-up includes:
- Blood tests for anemia and infection
- Tests for electrolytes
- Tests for pancreas and liver enzymes, to check these organs
- Pregnancy test
- Urine analysis, to test for infection or other urinary causes
- Drug screen, to test for drug-related reasons of vomiting
- X-rays of the abdomen, to check for conditions like blockage
- Upper endoscopy, to view the stomach and esophagus for possible causes of vomiting
- Head CT scan, if a nervous system cause of vomiting seems likely
- Abdominal CT scan, to check for health problems that might need surgery
Three Phases:
| Prodromal | Early morning nausea and abdominal pain |
| Hyperemetic | Ongoing nausea, repeated bouts of vomiting, abdominal pain, decreased food intake, weight loss, dehydration |
| Recovery | Starts when cannabis is stopped completely (variable time frame) |
Treatment:
The definitive treatment of Cannabinoid Hyperemesis Syndrome is discontinuing the causative agent (marijuana). Medical management, especially rehydration, is essential to prevent complications. Traditional antiemetic medications (ondansetron, metoclopramide, prochlorperazine, promethazine) are ineffective for active symptom relief. Research has shown Haloperidol and Lorazepam to be effective in relieving nausea/vomiting. Due to the persistent vomiting, gastritis and esophagitis may manifest. Often patients will also need a proton-pump inhibitor (omeprazole, pantoprazole, lansoprazole) for healing.
Patients with Cannabis Hyperemesis Syndrome compulsively take hot showers with reported relief of symptoms. The hypothesized mechanism of action is that hot water activates transient receptor potential vanilloid 1 (TRPV1) receptors, resulting in impaired substance P signaling in the area postrema and nucleus tractus solitarius. Another “dry” method would be to apply capsaicin cream to the abdomen. The topical capsaicin cream binds to TRPV1 receptors with high specificity, impairing substance P signaling, much like a hot shower.
If nausea/vomiting is severe and the patient is showing signs/symptoms of dehydration, hospitalization may be required as this is a life-threatening event.
Price SL, Fisher C, Kumar R, Hilgerson A. Cannabinoid hyperemesis syndrome as the underlying cause of intractable nausea and vomiting. J Am Osteopath Assoc. 2011 Mar;111(3):166-9. PubMed PMID: 21464265.
Smith TN, Walsh A, Forest CP. Cannabinoid hyperemesis syndrome: An unrecognized cause of nausea and vomiting. JAAPA. 2019 Apr;32(4):1-5. doi: 10.1097/01.JAA.0000554231.86747.0a. PubMed PMID: 30913155.
Book online securely or call (941) 500-9292

Recent Comments